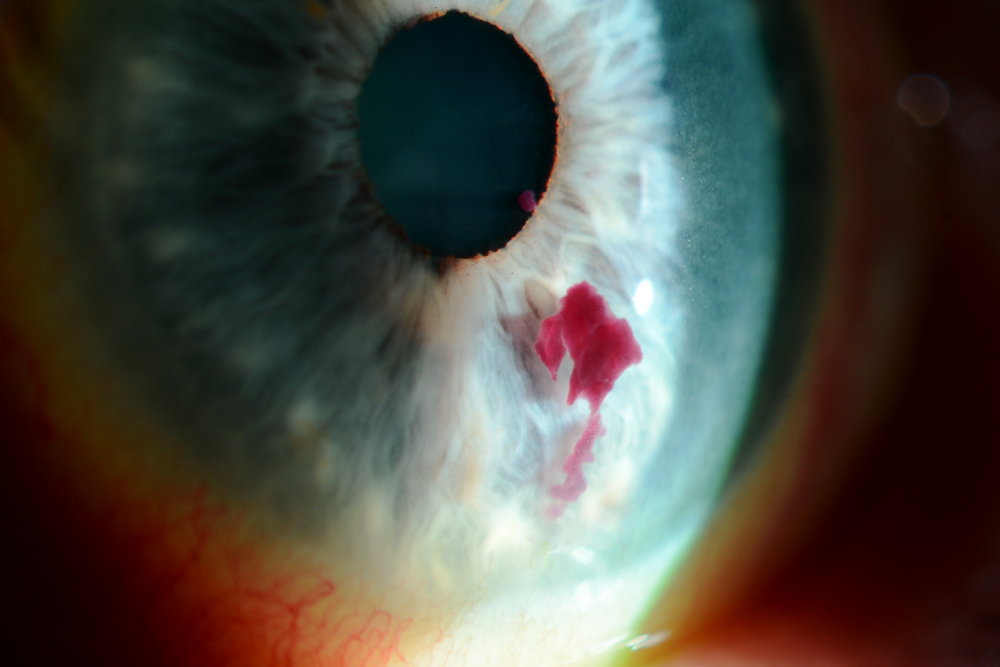
Dry eye and menopause: Understanding the connection
Keeler

Menopause is a significant transition in a woman’s life, marked by fluctuating hormones and various physical changes. While hot flashes, mood swings, and sleep disturbances are often discussed, one common yet lesser-known issue is dry eye syndrome. Many women experience discomfort in their eyes during menopause, often without realising the connection between hormonal changes and their eye health.
In this blog, we’ll explore why dry eye becomes more prevalent during menopause and how to manage this condition effectively. In addition to this blog, why not catch up on the Q&A with Nicola Bennett and Priya Udani that took place on World Menopause Day 2024.
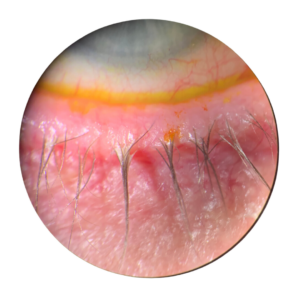
What is dry eye syndrome?
Dry eye syndrome occurs when the eyes do not produce enough tears, or the tears evaporate too quickly, leading to dryness, irritation, and inflammation. Tears are vital for maintaining the health of the eye’s surface and providing clear vision. When tear production decreases or their composition changes, the result can be uncomfortable symptoms like:
- Redness
- Itching or burning sensation
- Sensitivity to light
- A gritty feeling, as if something is stuck in the eye
- Intermittent blurred vision
While dry eye syndrome can affect anyone, women going through menopause are at a higher risk due to the hormonal changes that occur during this phase.
The link between menopause and dry eye
Menopause is characterised by a decrease in estrogen and progesterone levels, hormones that play a significant role in various bodily functions, including maintaining the health of the eyes. Here’s how these hormonal shifts contribute to dry eye:
1. Estrogen decline
Estrogen helps regulate tear production by influencing the meibomian glands, which secrete the oily layer of the tear film that prevents tear evaporation. When estrogen levels drop during menopause, these glands may not function optimally, leading to faster tear evaporation and drier eyes.
2. Testosterone and progesterone levels
Interestingly, testosterone, a hormone commonly associated with men but also present in women, contributes to tear production. As testosterone levels decrease during menopause, the eye’s ability to produce tears diminishes, exacerbating dry eye symptoms. Similarly, progesterone levels drop during menopause, which also impacts tear production and quality.
3. Environmental and lifestyle factors
In addition to hormonal changes, lifestyle factors such as prolonged screen use, air conditioning, diet and medications often used by menopausal women (like antihistamines and diuretics) can worsen dry eye symptoms. These factors further compound the discomfort caused by hormonal shifts.
4. Skin
As there is a decline in hormones over time, there is a change in the quality and composition of skin. Inflamed skin such as those with a rosacea skin type develop increase sensitivity exacerbating inflammation which fuels blepharitis and oil production from the meibomian glands resulting in chronic dry eye. Also with a loss of collagen from 1%/year to 30% when you hit perimenopause, there is a loss of elasticity and scaffold in the skin. This down south phenomenon can affect the position of the lower eyelids resulting in the inability of lids to meet on blinking or sleeping. This can result in exposure of the cornea and evaporation of the water part of the tear film.
Recognising dry eye symptoms during menopause
For women going through menopause, it’s essential to recognize the symptoms of dry eye early on. While symptoms like redness or irritation may seem mild, untreated dry eye can lead to more serious problems, such as eye infections or damage to the cornea over time.
- Pay attention to the following signs:
- Eyes feeling consistently tired or strained
- Difficulty wearing contact lenses
- Increased tearing (this can be the eye’s response to irritation)
- Difficulty reading or working on a computer for extended periods
If you notice these symptoms, it’s time to talk to an eye care professional who can help to diagnose dry eye and recommend an appropriate treatment plan.
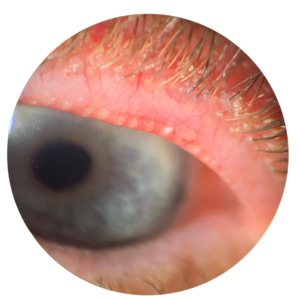
Managing dry eye during menopause
While dry eye can be uncomfortable, there are various strategies to help manage the condition. Here are some ways to reduce discomfort and protect your eyes:
1. Artificial tears and eye drops
One of the most common treatments for dry eye is the use of artificial tears. These over-the-counter lubricating eye drops can help maintain moisture on the eye’s surface. For more persistent dry eye cases, prescription-strength eye drops that increase tear production may be necessary.
2. Warm/heat compresses
Applying a warm compress over the eyes can help stimulate the meibomian glands and improve the quality of the tears by reducing inflammation and promoting better tear film stability. This should be done daily for 10 minutes, followed by a light lid massage and wash with an eye cleanser.
3. Omega-3 fatty acids
Dietary changes, such as increasing the intake of omega-3 fatty acids, may help improve tear production and reduce inflammation. Omega-3s are found in fish such as salmon, walnuts, and flaxseeds. Supplements are also available and can be beneficial if dietary intake is insufficient.
4. Hydration
Staying hydrated by drinking plenty of water is crucial for tear production.
5. Prescription medications
For severe cases of dry eye, an ophthalmologist may recommend prescription medications that either increase tear production or reduce inflammation of the eye’s surface. These treatments can provide longer-term relief when over-the-counter options are insufficient.
6. Punctal plugs
Punctal plugs may be an option. These tiny devices are inserted into the tear ducts to block drainage, allowing more tears to remain on the eye’s surface. This treatment can provide significant relief for women with chronic dry eye.
7. Low Level Light Therapy
Low-Level Light Therapy (LLLT) a non-invasive treatment that has gained popularity for managing dry eye syndrome, particularly among menopausal women. This therapy uses LED light, usually in the red or near-infrared spectrum, to stimulate the meibomian glands, which are responsible for producing the oily layer of the tear film. By enhancing gland function, LLLT can help improve tear quality and reduce symptoms associated with dry eye.
8. Intense pulse therapy and radio frequency
For the longest time IPL has been a standalone treatment for dry eye which really is restricted to Fitzpatrick skin types 1-4. The introduction of radiofrequency has changed the face of blepharitis treatment. The combination of the two work to heat the meibomian glands to the correct temperature with the RF for a much better expression of the glands and the stimulation of collagen formation to reignite those scarring over glands and the IPL eradicates the demodex as well as treats the new inflamed telangiectasia vessels.
There are a whole host of products now available on the market to support patients with dry eye and blepharitis from clean eye make up for sensitive eyes, to lid scrubs containing okra and manuka honey eye drops for lubrication. Dry eye is so debilitating and when these patients attend a hospital service they have tried every drop under the sun and have used warm compresses and there is just no relief. We are only really beginning to understand the complexity of dry eye and it’s multifactorial causes but dry eye is now a recognised disease and by increasing awareness and treating it sooner we may be able to save a lot of patients the heartache that comes with dry eye.
The importance of regular eye exams
Sarah Farrant MCOptom, at Earlam and Christopher, Taunton, Somerset, has a special interest in dry eye disease (DED). “We encounter women with DED all the time… we do see many more women coming in with dry eye than men, especially in their 40s and 50s.”
If you’re approaching menopause or are already experiencing symptoms, regular eye exams become even more important. Your eye doctor can monitor changes in your eye health and suggest timely interventions to prevent dry eye from worsening. In many cases, a comprehensive eye exam will reveal underlying dry eye issues, even if symptoms are mild.
Conclusion
Menopause brings many changes, and while dry eye syndrome may seem like a minor inconvenience, it’s important to address it early to prevent complications. Understanding the link between menopause and dry eye can empower women to take proactive steps toward maintaining eye comfort and health. With the right treatments and lifestyle adjustments, dry eye doesn’t have to be a persistent problem during this transitional phase of life.
If you’re experiencing dry eye symptoms during menopause or even before starting HRT, don’t hesitate to reach out to an eye care professional to discuss the best options for relief.
We’d like to thank Ms Priya Udani (BSc honors, MBBS, FRCOphth) Consultant Oculoplastic Surgeon, Dry eye specialist and Aesthetic Doctor, and Ms Sarah Farrant MCOptom, at Earlam and Christopher, Taunton, Somerset and Hamza Mussa, Senior Optometrist, for their contributions to this blog post.